Navigating Strep Throat with Knowledge and Care
Ouchy throat…? Is it just a sore throat or could it be Strep?
A scratchy, painful throat can put a damper on anyone’s day. But with so many potential causes, figuring out what’s behind your child’s discomfort can feel like a mystery. In this blog post, we’ll unravel the intricacies of strep infections, exploring the potential complications, preventive measures, and the crucial role of parental vigilance.
The Common Culprit:
A sore throat is a symptom, not a specific illness. It can be caused by a variety of factors, including:
-
- Viruses: The most common cause, responsible for up to 90% of sore throats. These include the common cold, flu, and mononucleosis.
- Irritants: Dry air, smoke, dust, and allergies can all irritate the delicate tissues in your throat.
- Bacterial infections: While less frequent than viruses, strep throat is the most well-known bacterial culprit and is most common in the school-age child.
- Other causes: Acid reflux, overuse of voice, and even certain medications can contribute to a sore throat.
Understanding Strep Infections:
Strep infections are primarily caused by the Group A Streptococcus pyogenes bacteria, with strep throat being a prevalent manifestation in children. Strep throat is more common in children than adults. It is most common in children 5 through 15 years old. It is very rare in children younger than 3 years old.
Signs and Symptoms: Unmasking the Culprit
Recognizing the early signs and symptoms of a strep infection is paramount for timely intervention. Watch out for:
-
- Sore throat
- Painful swallowing
- Fever > 38 degrees Celsius and chills
- Red and swollen tonsils
- Headache
- Rash (in the case of Scarlet Fever)
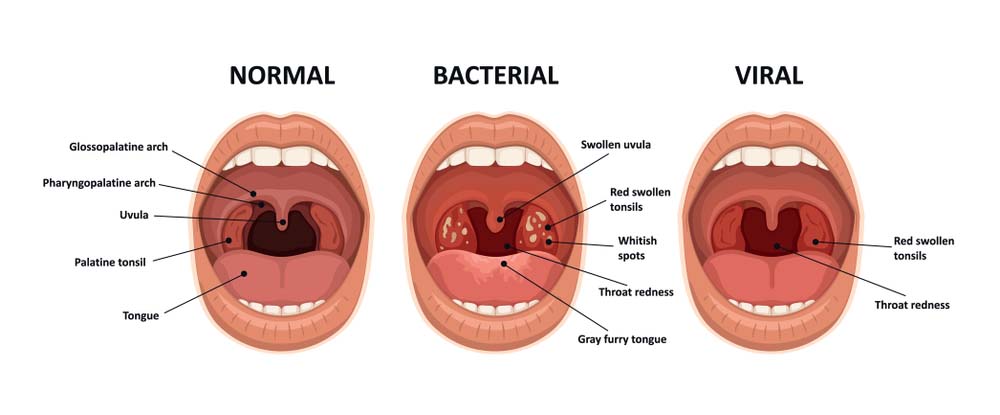
Differentiating Strep from Viral Infections;
Keep an eye out for:
- Sudden onset: This can be a red flag. Strep comes in suddenly and quickly unlike viral infections which set in gradually over several days.
- Absence of cough/runny nose: While not definitive, strep often lacks these cold-like symptoms.
- White spots or patches on tonsils: A telltale sign, but not always present.
Less common symptoms may include:
-
- Headache
- Stomach pain
- Nausea or vomiting (more common in young children)
- Strawberry tongue (a red and bumpy tongue)
- Rash (scarlet fever) Red rash that feels rough like sandpaper. One to 2 days after the illness begins, a red rash usually appears. However, the rash can appear before illness or up to 7 days later. Skin peeling as the rash fades.
Symptoms do NOT usually include cough or runny nose
The following symptoms suggest a virus is the cause of the illness instead of strep throat:
-
- Cough
- Runny nose
- Hoarseness (changes in your voice that make it sound breathy, raspy, or strained)
- Pink eye (conjunctivitis)
Strep Throat Contagion
Strep throat is a highly contagious disease that can spread rapidly among groups and family members if not quickly diagnosed and treated with antibiotics.
Kids can get strep throat from being very close to other kids, from sharing food and drinks or coming into contact with saliva or nasal secretions from someone who has strep. Kids are generally no longer contagious after taking antibiotics for 24 hours and can return to school.
Families can help reduce the spread of strep throat by:
-
- Frequent handwashing
- Not sharing food or drinks
- Staying home and avoiding close contact with others when you are sick
- Taking your child to the doctor if you think they may have strep
Diagnosing Strep Throat
Appropriate treatment and prevention of infection spread hinge on the ability to diagnose strep throat accurately. A rapid strep test and a throat culture are the two most common tests for this purpose.
Diagnosing strep with a rapid strep test
The rapid strep test is designed to detect strep A antigens, substances that elicit an immune response. During this test, a cotton swab collects bacteria from the tonsils and back of the throat. The test typically takes 5-10 minutes after sample collection.
Diagnosing strep with a throat culture
A throat culture is a more detailed and specific test for strep that is performed in a lab. If the rapid test is negative, the doctor may send the culture to the lab for processing.
In the Kenyan setting, where Rapid Group A Strep Ag test may not be widely available in an office practice, it is also common to do a full blood count. This test does not specifically identify Streptococcus pyogenes but does help distinguish between a bacterial or viral infection.
Treatment Approaches: Navigating the Antibiotic Route
Antibiotics are the cornerstone of strep infection treatment, aiming to eliminate the bacterial culprit. Commonly prescribed antibiotics include penicillin or amoxicillin. Antibiotics to treat Strep are given for 10 days. It is crucial to complete the entire course, even if symptoms alleviate, to prevent bacterial resistance and potential complications.
-
- Pain Relief: Over-the-counter pain relievers like paracetamol or ibuprofen can ease discomfort and reduce fever.
- Rest and Hydration: Adequate rest and hydration play a pivotal role in recovery, supporting the body’s immune response.
Antibiotics will help alleviate symptoms by about a day, but more importantly help prevent spread of the infection and prevent serious complications of Strep. Kids are generally no longer contagious after taking antibiotics for 24 hours and can return to school.
Acute Rheumatic Fever is a complication of Strep infection. If your child doesn’t receive treatment or doesn’t complete treatment, their immune system may attack its own tissues. The bacteria is thought to trick the body’s immune system into attacking healthy tissue. This usually happens in the heart, joints, skin and central nervous system. This incorrect immune system reaction causes swelling or inflammation of joints and tissues in the heart, skin, and brain.
It mostly affects children and teenagers (ages 5 to 15). Rheumatic fever usually develops two to three weeks after an untreated strep throat or scarlet fever infection. Rheumatic fever generally doesn’t occur in children younger than 5 years and older than 15 years.
Common rheumatic fever symptoms include:
-
- Swollen, tender and red joints (arthritis) — especially your child’s knees, ankles and elbows — that may move around from day to day (called migratory pains)
- Jerky movements your child can’t control in their hands, feet or other body parts (chorea).
- Small bumps (nodules) under your child’s skin.
- Chest pain or abnormal heartbeat.
- Feeling overly tired all the time (fatigue)
- Fever
One complication of rheumatic fever is long-lasting heart damage. This is called rheumatic heart disease. Rheumatic heart disease usually occurs years to decades after the original illness. However, severe rheumatic fever can start to damage the heart valves (most commonly the mitral valve) while a child still has symptoms of the infection. Heart damage from rheumatic fever may cause permanent damage to heart valves, irregular and fast heart beats (arrhythmia) later in life, as well as heart failure. Rheumatic heart disease is the most common cause of acquired heart disease in young people around the world.
Children who have had Rheumatic Fever are at increased risk of getting it again. To prevent this from happening, they are put on a prolonged course of antibiotics, given on a monthly basis for 5-10 years or until they reach the age of 21 years.
Acute glomerulonephritis (AGN) is a kidney disorder resulting from the immune system’s response to infection, and strep throat is a significant trigger. The infection can lead to inflammation in the glomeruli, the tiny filters within the kidneys responsible for removing waste and excess fluids.
The Strep-AGN Connection: Recognizing the Signs
Following a strep infection, signs of acute glomerulonephritis may not immediately manifest. It’s crucial for parents and caregivers to be vigilant for:
-
- Dark urine
- Swelling (edema), particularly around the eyes or in the ankles
- High blood pressure
- Fatigue
- Decreased urine output
Risk Factors: Who’s at Greater Risk?
Certain factors increase the likelihood of developing AGN after a strep infection:
-
- Age: Children between 6 and 10 years are more susceptible.
- Type of Strep Infection: Certain strains of streptococcal bacteria, like those causing skin infections, carry a higher risk.
- Genetic Predisposition: A family history of AGN may elevate the risk
Conclusion
Strep infections, though common, should not be underestimated. Being proactive in recognizing symptoms, seeking timely medical attention, and understanding potential complications empowers parents to safeguard their children’s health. By staying informed and actively participating in their healthcare journey, parents can effectively navigate the complexities of strep infections and ensure their little ones thrive in good health.





